If you’ve been denied your Internal First-Level of Appeals, then the next step in the game is your Internal Second-Level of Appeals. This is typically your last chance to prove your case within your insurance company before you have to submit for an external review with your state’s Department of Insurance.
In this level of the appeals process, the appeal is typically reviewed by a medical director/reviewer panel at your insurance company who was not involved in the initial claim decision. This is your chance to prove your case to a new panel of reviewers.
The goal of this appeal is to prove that the requested DME should be accepted within the coverage guidelines. Just as with the First-Level of Appeals – you need to prove that the requested DME meets your insurance company’s definition of “MEDICAL NECESSITY.”
This is where you will have the opportunity to write your own letter to the appeals board, submit all the prior information your medical professional submitted again, and add any addendum’s to prove “medical necessity” for requested DME.
Note:
This process is a little bit more involved in that the insurance appeals team normally consists of a medical director, several physicians who “claim” to have expertise in physical rehabilitation, and perhaps a medical coder.
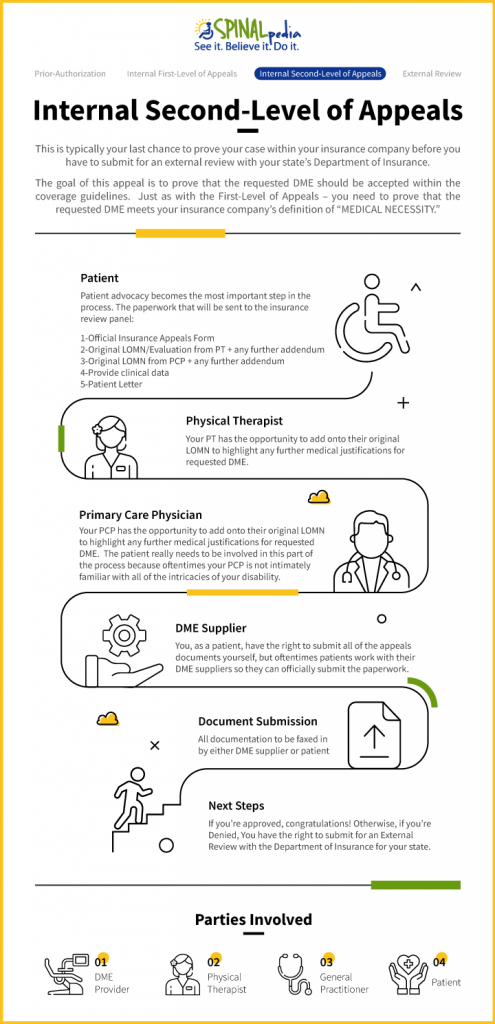
How Does the Internal Second-Level of Appeals Process Work?
Parties involved for Second-Level of Appeals:
- Durable Medical Equipment (DME) Provider
- Physical Therapist (PT)
- General Practitioner and/or other Medical Professional (PCP)
- Patient
Second-Level of Appeals Flow:
- Patient needs to read all of the denial paperwork to determine why the insurance company denied the piece of DME.
- If the DME was denied because it was not classified as “medically necessary” under your insurance policy then:
- You, your PCP, or DME provider will fill out a standard Members Appeals Form & submit the following information:
- PCP previous Letter of Medical Necessity (LOMN) + addendum further justifying why requested DME is “medically necessary” for the patient.
- PT Previous LOMN/Evaluation + addendum further justifying why requested DME is “medically necessary” for the patient.
- Patient personal letter to appeals team explaining your history, story, disability, and how requested DME improves quality of life and daily living activities in the home. If you can provide pictures of why requested DME is critical for your in-home care; this can be very useful because visuals are always helpful.
- Typically your DME provider will be able to gather all the paperwork from you and submit your Second-Level Appeals to your insurance. However, as a patient, you have the right to gather all the paperwork yourself, and submit to insurance.
- If you do have your DME provider submit your paperwork make sure to look it over before final submission.
Note:
- Your insurance company may not agree with your medical professionals definition of “medically necessary” as defined by your insurance companies’ benefit limitations and exclusions in your policy.
- However, it’s important to note that even if you are denied during the First-Level of Appeals you do have the ability to make your case why an exception should be made in your particular medical circumstance again during the Second-Level of Appeals.
- This is really the time to throw the kitchen sink of paperwork at your insurance company because this is your last level of internal appeals before you have to submit for an external review to try and go above your insurance company’s head if they deny you.
Timeline Expectations

Tips & Tricks #1: Organization
- Organization is Key. There are many pieces of the puzzle during the appeals process. Make sure to keep calling and emailing your medical professionals and DME companies to follow up, so they submit all the paperwork together and in a timely manner.
- Be sure to proofread all medical professionals LOMN’S prior to submitting to insurance to make sure they properly cover all medical conditions with respect to why requested equipment is “medically necessary” in your everyday life.
- You are in control and it is your responsibility to make sure all paperwork is complete. They will respect what you inspect. These companies work for you, not the other way around.
Be Pleasantly Persistent. Persistence is key when winning insurance battles. Make sure to take detailed notes of all emails, phone calls, and keep paperwork throughout the process.
Patient Responsibilities

The Second-Level of Appeals is really where patient advocacy becomes the most important step in the process since this is your last chance to try and have your DME approved through the internal appeals process of your insurance company.
If you remain organized throughout the Prior-Authorization and the First-Level of Appeals, then you will really focus on writing your own personal letter to the insurance appeals panel.
As discussed in previous sections, but it is worth reiterating, during the Second-Level of Appeals the paperwork that will be sent to the insurance review panel, a different review board from the First-Level of Appeals, includes:
-
Official Insurance Appeals Form: Generally filled out by your DME, but patients can take responsibility for this as well.
-
Original LOMN/Evaluation from PT + any further addendum to further justify requested DME’s “medical necessity.”
- It’s best to send an email or call your PT to see if they can offer any further written justification why the requested DME is so important in your life, medically necessary, and unique to your specific medical condition.
-
Original LOMN from PCP + any further addendum to justify requested DME’s “medical necessity.”:
- Just as with your PT, it’s a great idea to call your PCP to see if they can add in any other medical language to justify approval for requested DME.
- Also, ask if your PCP will call your PT to coordinate language between the letters. If they will not, then request to see both letters from your PCP and PT to cross-reference one another to see if any changes need to be made.
-
Provide clinical data, such as published journal articles or data on outcomes on the clinical and/or therapeutic benefits of requested DME.
- This is not always available, but throwing in the “kitchen sink” of paperwork at this level of the game is necessary. See if you can dig around the internet to find any journal articles or papers to further your case.
- If you can’t find anything on your own, consider contacting the manufacturer of the requested DME to see if they have any studies or papers justifying the medical necessity & benefits of the DME.
-
NOTE: This step can take a lot and can be challenging, but if you can find anything at all from a third party source on how requested DME provides therapeutic benefits – it can only help your case!
-
Patient Letter: This is REALLY IMPORTANT. This is where you have the chance to stand out to the review panel. You want this letter to contain the following elements:
- Your name, personal contact information, medical condition, medical history, and specific health issues.
- Reasons why requested DME is “medically necessary” for in-home use in your life.
- Tell the review board about your story and struggles in life.
-
NOTE: While the review board does not make medical decisions based on your life story you are trying to humanize yourself to not just be a number in a file. You never know what might strike a review board, so pulling at the heartstrings is helpful in some circumstances.
Helpful Resources:
You may not know how to write a personal letter, but you now understand all the components that go into it.
The Cystic Fibrosis Organization has put together an incredible document regarding understanding the appeals process for all kinds of medical conditions. In particular on page 18 and below there are three different sample letters that can be tailored to be written by your doctor or yourself. Essentially you fill in the red areas.
There’s no need to recreate the wheel when an organization puts together a great document – this document deserves recognition, and will be incredibly helpful for you.
Click Here to check out the sample letters (don’t forget to turn to page 18 first) – remember to add in your personal story.
To help you better understand different expectations, requirements, and tips for assisting your medical professionals write the best LOMN’s for you – here are some examples:
There are dozens of other websites out there, but these should get you started and familiarized with proper templates, advice, and tips for LOMN’s.
Tips & Tricks #2: Patient Recommended Responsibilities
- Since this is your last shot at an internal appeal with your insurance company you want to make sure you submit as much information as you possibly can.
- For example, if your PCP wrote just one or two paragraphs for your LOMN during your First-Level of Appeals, then sit down and chat with them about writing a further page on why requested DME is “medically necessary” in your home. Ask your PCP to re-read what your PT wrote on their LOMN/Evaluation to try and use the same language.
- To make this point crystal clear – for example, if you are trying to get a seat elevator approved for your power wheelchair; you, your PCP or PT may have just written that the seat elevator allows you to get up to your sink to perform daily hygiene duties.
Think critically about what else the seat elevator can do in your home such as help you raise up to the microwave to cook food, open your front door, raise up to a desk to get to work, etc. Details are absolutely key.
- Make sure that your personal letter to your insurance company clearly outlines your personal history, disability, and approaches the need for requested DME from a “patient” perspective. Oftentimes your medical professionals just state the “medical necessity” of the requested DME, but offer the appeals panel your personal story.
- Every perspective helps. For example, your medical professionals may not understand that when you’re in your home you cannot reach the double stack laundry machine by yourself without a seat elevator. If you don’t have round-the-clock caregiving, tell them why it is so important that you be able to raise your chair up to do laundry yourself. Show them that you are a person with real needs and not just a number in a case.
- Finally, if you are able to take pictures along with your personal letter of why requested DME is medically necessary, this is your chance to do so. For example, you are trying to get a seat elevator approved and your bed height is too high and you need to raise your chair up for a safe & level transfer; take a picture of how low your wheelchair is compared to your bed height. A picture is worth a thousand words.
Physical Therapist Responsibilities

As mentioned previously, your PT is going to be your biggest advocate when specifically trying to have DME approved for in-home use. However, not every patient has a competent PT or a PT at all. If this is the case, then you just need to work more closely with your PCP on Letters of Medical Necessity (LOMN)
During the Second-Level of Appeals your PT has the opportunity to add onto their original LOMN to highlight any further medical justifications for requested DME.
Finally, your PT will then fax back the documentation to your DME supplier before submitting back to your insurance company.
Primary Care Physician Responsibilities
During the Prior-Authorization phase of the process your PCP will have submitted a Letter of Medical Necessity (LOMN) on your behalf trying to justify why the requested DME is “medically necessary” with your medical condition. Ideally this letter will have echoed your PT’s in a similar manner.
During the Second-Level of Appeals your PCP has the opportunity to add onto their original LOMN to highlight any further medical justifications for requested DME. The patient really needs to be involved in this part of the process because oftentimes your PCP is not intimately familiar with all of the intricacies of your disability.
It is really best to try to make another appointment and brainstorm further medical justifications for requested DME.
DME Supplier Responsibilities
There really is not too much for your DME supplier to do at this stage of the game except for organization.
You, as a patient, have the right to submit all of the appeals documents yourself, but oftentimes patients work with their DME suppliers so they can officially submit the paperwork.
If your DME supplier does handle sending in your appeals paperwork to your insurance company, make sure the following gets completed, and in a timely manner:
- Official insurance appeals form is filled out
- Patient personal letter
- PT original LOMN/Evaluation and any additional documentation
- PCP original LOMN and any additional documentation
- Clinical data or published journal articles if applicable
- DME supplier quote for requested DME
Many of these pieces of the puzzle can get lost in the mix and left out when faxing over to your insurance company.
As a patient you need to make sure to double check all of the work before they fax it over, especially if you’re working with a national DME company.
Submission
Documents to be submitted:
- DME Supplier or patient to fill out Level 2 Members Appeals Form, which can be found on insurance website portal or by calling customer service.
- PT Paperwork (Original LOMN/Evaluation + Addendum if applicable)
- PCP Paperwork (Original LOMN + Addendum if applicable)
- Clinical Data paperwork if applicable
- Patient Personal Letter
All documentation to be faxed in by either DME supplier or patient.
Tips & Tricks #3: Stay One Step Ahead of the Game
It’s always a great idea to stay one step ahead of your insurance company. What we mean by that is that it’s important to anticipate a denial. If you are denied and have exhausted all of your internal appeals rights then you have the option to submit for an external review to your State’s Department of Insurance.
This is a great step, but you can take it one step further. If you are, in your opinion, unjustly denied a piece of DME that is “medically necessary,” you have further rights than to just submit an external review. You have the ability to:
- Reach out to your Local Legislators
- Hop on Google and find out who your Local Legislators are, their contact information, and be prepared to call them if you are denied.
- Prepare emails and letters ready to send out if you are denied the Second-Level of Appeals
- Reach out to your Local Investigative Reporters in the News
- Hop on Google to research your local TV stations, who the investigative reporters are for healthcare injustices, etc. You can even call the TV station to get the names of the people you need to reach out to.
- Prepare emails and letters ready to send out if you are denied the Second-Level of Appeals
It’s always a great idea to hope for the best, but plan for the worst.
If you exhaust your internal appeals then you have the right to submit an External Review, reach out to your Legislators, and try and see if a Local Investigative Reporter will take your story.
Insurance companies do not like bad press. Therefore, you have to approach a denial from all angles in order to change their mind. Unfortunately, insurance companies don’t really care about you, so you have to make them accountable for their actions.
Next Steps
If you’re approved, congratulations!
If you are denied the Internal Second-Level of Appeals, then you have exhausted all of your insurance company’s internal levels of appeal rights.
At this stage of the process you have one more option to try and have your requested DME approved. You have the right to submit for an External Review with the Department of Insurance for your state.
Effective January 1, 2012, health insurance issuers in all states must participate in an external review process that meets minimum consumer protection standards as outlined by the Affordable Care Act.
You will submit all the same paperwork you submitted for the internal Second-Level of Appeals for your insurance company in addition to any other supporting documentation you can think of.
Your States Department of Insurance is conducted by an independent, third-party reviewer in collaboration with the physician who is board certified in the same specialty as the patient’s physician.
In the proceeding sections we will walk you through all of the steps you need to take to submit for an external review, what you will need, supporting documentation, and links.
Note:
We will also be discussing alternative steps you can take if the requested DME is not covered under your plan benefits such as reaching out to your legislators, local news outlets, and investigative reporters.




