If you have been denied by your insurance company for the Second-Level Internal of Appeals, you’ve now exhausted all of your internal appeals rights. The last step in the process is to submit an external review with your state’s Department of Insurance (DOI)
After all the work you’ve completed so far, it can be extremely discouraging knowing that you have no more rights within your insurance company to fight for the requested DME you, and your medical providers have tried to justify is “medically necessary” for your disability.
Don’t lose hope yet though as you have one more shot with your external review in addition to going above and beyond reaching out to your local legislators and local media.
There are two steps in the external review process:
The DOI consists of a panel of independent reviewers who are supposed to have a specialty in the area of your disability.
When filing an external review you can also request an expedited review if requested DME is urgent for in-home care.


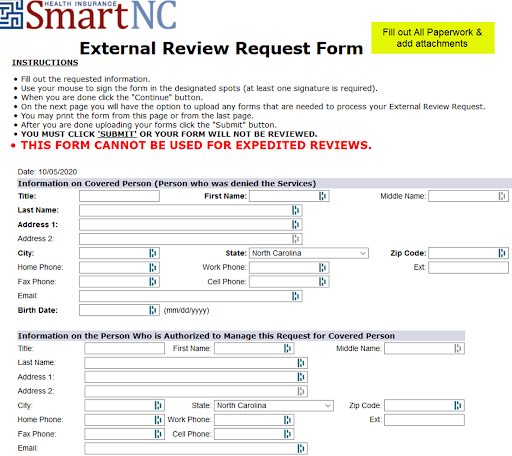
NOTE:
Since this is your last chance to plead your case for requested DME it is best to throw in the kitchen sink and then some. (i.e. photographs of how requested DME improves your life within your home, further letters explaining why requested DME is so crucial to your daily life, improves your assisted daily living activities, and makes you more independent.

Patient responsibilities during an external review are a bit more cumbersome during this stage of the process because while you can have a medical professional submit documentation on your behalf, it’s really in your best interest to submit all documentation online or send in by mail yourself.
The reason being is you want to collect all of your:
This can be a lot of paperwork to send in, but throughout the entire insurance process you want to make sure to have a physical folder with all of the documentation or stored somewhere on line as you go.
Also, since you have multiple medical professionals who will be involved in the process it’s highly doubtful they will have all of your documentation in one location and send in everything in its entirety.
During each phase of the denial process it’s best to create a folder titled, for example, “Prior-Authorization,” or “First-Level of Appeals.” This way you have all of your paperwork organized, and it won’t seem as daunting when you have to submit it to the Department of Insurance for an External Review.
However, you only get one shot at this so you want the Department of Insurance to not only have all of the facts, but plead your case further so they can overturn your insurance company’s final denial decision.
You are really in the driver seat on this one, so be organized, stay upbeat because by this stage of the game you likely have been through quite a lot, are exhausted, frustrated, but don’t give up yet!
Tips & Tricks #1: Patient Tips
If you are given a final denial by the Department of Insurance the disappointment level can definitely be high. It may appear as if you have exhausted all of your rights, but as mentioned in previous steps above, you still have a few cards to play.
The three main avenues you have at your disposal are:
Lastly, even if you are denied a piece of equipment that you and your medical professionals think is medically necessary, but your insurance company disagrees with you … You are taking the first step to change the system.
It all comes down to a great number of people getting together to change policy. Many people may not be up for this, which is fine, but if you are one of those who want to take things a step further to make systemic changes in the healthcare system – it always starts with one person.
Rome was not built in a day as they say. With respect to medically necessary equipment, ponder this for a moment:
Many years ago the tilt function on a power wheelchair was not considered medically necessary for the severely disabled. After many thousands of disabled folks, lawyers, physical therapists, and other advocates in the community put a great deal of money into clinically proving that weight shifting back in your wheelchair prevents pressure sores, thus reducing long-term healthcare costs for insurance companies – Medicare, where most policy shifts start, deemed the tilt function on power wheelchairs is medically necessary.
Change has to start somewhere, and if you are really interested in advocacy, just keep going by any means necessary whether that be working with your elected officials, creating social media campaigns to change the system, or working with your local media outlets.

While you are waiting for a decision from the Department of Insurance on your case it is a good idea to familiarize yourself with all of your Federal, State, and Local Legislators.
If you are denied by the Department of Insurance, the next step of the game is to reach out to your Elected officials to see if they can help you, and if you have a case to find a loophole within your insurance policy or whether or not your final insurance decision was just for your medical situation.
If you have all of this information prepared, then if you are denied, you can start taking action right away, and have the right people in your corner to help you.
Click here to find your Elected officials.
Tips & Tricks #2: Elected Officials Tips
Most importantly, don’t give up!

After you have exhausted all of your internal level of appeals with your insurance company and while you’re waiting for your Department of Insurance external review it’s a great idea to start gathering a contact list of your local media investigative reporters.
Insurance companies generally do not like negative publicity and if you have a real case, and even if the Department of Insurance denies your claim, oftentimes having your story put out there in the local media has an interesting way of changing an insurance company’s final decision.
This process can seem a little bit daunting, but the best way to go about it is to:
Tips & Tricks #3: Local Media Tips
The biggest piece of advice we can offer you is to be pleasantly persistent and aggressive when reaching out to your local media because there are always dozens of stories each day they have to choose between.

SPINALpedia
